Targeted MRI-US fusion biopsy is an emerging technology with the potential to change the standard of care for diagnosis and treatment. It combines the accuracy of MRI with the real-time monitoring of ultrasound to detect more clinically significant cancer, while preventing unnecessary biopsies. Unlike standard systematic biopsy, fusion can track lesions over time with imaging or repeat biopsy during active surveillance. According to a national survey, about 86% of urologists agree that MRI is a valuable tool, yet only 60% use MRI for fusion biopsies. 24% of urologists agree fusion should be the standard of care, while 65% believe it should be reserved for special cases like an elevated PSA and prior negative biopsy. Although transition to fusion has been slow, 67% of participants agreed it had become more popular over the past 5 years.1 The demand for MRI-targeted biopsies will continue to grow as the supporting literature develops and the technology becomes more accessible. Currently, there is an opportunity for imaging centers to bridge the gap between knowledge and accessibility for urology practices.

Implementing a new technology often requires significant resources and comes with additional barriers. 60% of urologists reported working for an institution or group with the resources to perform MRI-US targeted biopsies. This varied between the types of practices, where 65% of solo practices struggled the most to utilize fusion and academic centers the least (30%).

On average, about 50% of the urology practices, mainly academic centers, in the US have the means to offer fusion biopsies. With current Medicare reimbursement, urologists would initially lose money by performing fusion because the payable amount is the same for a standard or fusion biopsy. Unfortunately, this means practices would have upfront costs, longer procedural times and would only get a return on investment once treating the cancer. In the long run, it is better for urology practices to adopt fusion, but for the 50%+ lacking the upfront capital, imaging centers could provide an appealing stopgap.

Without the immediate financial incentive, most urology practices are unable to afford or justify the cost of acquiring the technology. Instead the kickback goes to imaging centers like provider-based joint ventures, ambulatory surgical centers (ASC) and more commonly, independent diagnostic testing facilities (IDTF) for performing the MRI. About 40% of the total imaging volume in the US is performed at IDTFs, while hospitals see 60%. Although the trend continues to shift towards IDTFs, the current number of prostate MRI requisitions is quite limited to the non-hospital practices with access to a fusion biopsy system. By integrating fusion, imaging centers can turn the cost barrier into an incentive for the majority of practices and ultimately drive the volume of prostate MRIs.
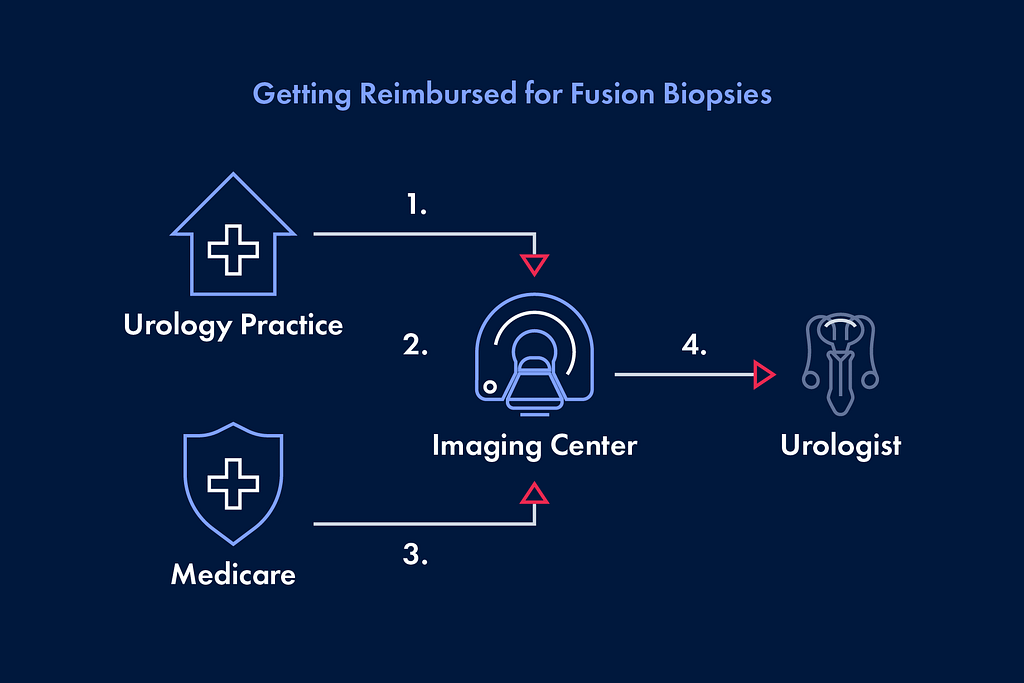
Getting Reimbursed for Fusion Biopsies
- Urology practices direct patients and urologists to imaging center for MRI-targeted fusion biopsies.
- Imaging center provides mpMRI scan, and reading and contouring of MRI.
- Medicare reimburses imaging center for all services including the MRI and biopsy procedure. The additional revenue may be up to $2500 per biopsy, depending on the setting and urologist/ radiologist payment structure.
- Visiting urologists are paid a fixed amount for performing fusion biopsies with the Fusion Bx 2.0.
Offering a lower cost setting, convenience and urologist incentive, imaging centers will see more patients and higher revenues as practices continue to adopt fusion. For more information about integrating fusion, please contact us at [email protected].
Get the full document below
* Revenue estimated based on ASC setting, including physician payment.
The 2022 National Average Medicare physician payment rates have been calculated using a 2022 conversion factor of $34.6062. Rates subject to change. Centers for Medicare and Medicaid Services. Medicare Physician Fee Schedule Look-Up Tool- updated April 01 2022. https://www.cms.gov/medicare/physician-fee-schedule/search
1 Tooker, G. M., Truong, H., Pinto, P. A., & Siddiqui, M. M. (2019). National survey of patterns employing targeted MRI/US guided prostate biopsy in the diagnosis and staging of prostate cancer. Current Urology, 12(2), 97–103. https://doi.org/10.1159/000489426
2 Levin, D., & Janiga, N. (2020, August 6). 2020 Outlook: Diagnostic Imaging Centers and Radiology Practices. HealthCare Appraisers. Retrieved from https://healthcareappraisers.com/2020-outlook-diagnostic-imaging-and-radiology-practices/